What is Spinal Stenosis?
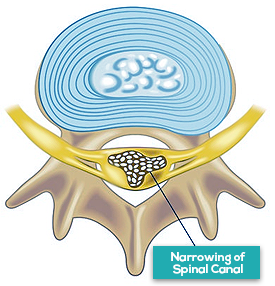 The narrowing of spaces between your spine is called spinal stenosis. This can add pressure to the nerve that travel through your spine. The condition is most common in the lower back and neck.
The narrowing of spaces between your spine is called spinal stenosis. This can add pressure to the nerve that travel through your spine. The condition is most common in the lower back and neck.
Sometimes spinal stenosis shoes no symptoms. On the other hand, some people have reported pain, tingling, numbers and muscle weakness. These symptoms may worsen over time.
Spinal stenosis is caused by wear-and-tear, also known as osteoarthritis. Wear and tear normally occurs during the natural aging process. However, this can also occur in younger people from an injury or trauma.
There are a couple different types of spinal stenosis, such as:
- Cervical Stenosis. This refers to the narrowing occurring in the neck.
- Lumbar Stenosis. In this condition, the narrowing occurs in the park of your lower back. This is the most common type.
Symptoms & Signs of Spinal Stenosis:
It’s normal for spinal stenosis to show up on imaging from an MRI or CT scan but without symptoms. Although when symptoms do occur, they will slowly increase over time. Nerves can also be affected depending on where the stenosis is located.
Cervical Stenosis (located in neck):
- Numbness or tingling in a hand, arm, foot or leg
- Weakness in a hand, arm, foot or leg
- Problems with walking and balance
- Neck pain
- In severe cases, bowel or bladder dysfunction (urinary urgency and incontinence)
Lumbar Stenosis (located in lower back):
- Back pain
- Numbness or tingling in a foot or leg
- Weakness in a foot or leg
- Pain or cramping in one or both legs when you stand for long periods of time or when you walk, which usually eases when you bend forward or sit
Causes & Risk Factors:
Most spinal stenosis occurs when something happens to that narrows the space of the open spine. Such as:
- Bone overgrowth. Wear and tear damage from osteoarthritis on the spine bones can prompt the formation of bone spurs. These can grow in the spinal canal. Paget’s disease, can also can cause bone overgrowth in the spine.
- Herniated discs. The soft cushions that act as shock absorbers between your vertebrae tend to dry out with age. Cracks in a disk’s exterior may allow some of the soft inner material to escape and press on the spinal cord or nerves, creating a herniated disk.
- Thickened ligaments. The tough cords that help hold the bones of your spine together can become stiff and thickened over time. These thickened ligaments can bulge into the spinal canal.
- Tumors. Abnormal growths can form inside the spinal cord, within the membranes that cover the spinal cord or in the space between the spinal cord and vertebrae. These are uncommon and identifiable on spine imaging with an MRI or CT.
- Spinal injuries. Car accidents and other trauma can cause dislocations or fractures of one or more vertebrae. Displaced bone from a spinal fracture may damage the contents of the spinal canal. Swelling of nearby tissue immediately after back surgery also can put pressure on the spinal cord or nerves.
It’s common to develop spinal stenosis when you are over the age of 50.
Risks factors that should be considered, are those who have:
- A spinal deformity
- Scoliosis
- A genetic bone disease
Treatment Options:
Depending on the location of the stenosis will also determine the treatment. The severity will also play a key factor in this.
If your symptoms are mild or you are not experiencing any, your doctor will likely recommend monitoring the situation. However, if it is more severe your doctor could recommend the following:
Medications
Your physician may prescribe medications, such as:
Pain relievers. Pain medications such as ibuprofen (Advil, Motrin IB, others), naproxen (Aleve, others) and acetaminophen (Tylenol, others) may be used temporarily to ease the discomfort of spinal stenosis.
antidepressants. Nightly doses of tricyclic antidepressants, such as amitriptyline, can help ease chronic pain.
Anti-seizure meds. Some anti-seizure drugs, such as gabapentin (Neurontin) and pregabalin (Lyrica), are used to reduce pain caused by damaged nerves.
Physical Therapy
Physical therapy may be recommended for those with spinal stenosis. It’s important to get back to a full range of motion. Patients often cease exercising due to the pain, however, it can actually help relieve pain if done properly.
Steroid Injections
It’s common for patients experiencing this condition to receive injections. A steriod injection can help reduce inflammation, therefore, reducing pain as well.
Decompression
This procedure is done by removing a portion of the thickened ligament. This is only performed for those who have a thickened ligament and lumbar stenosis.
Surgery
Surgical options might be considered if other treatments have failed. Surgies include the following:
-
Laminectomy. This procedure removes the back part (lamina) of the affected vertebra. A laminectomy is sometimes called decompression surgery because it eases the pressure on the nerves by creating more space around them.
In some cases, that vertebra may need to be linked to adjoining vertebrae with metal hardware and a bone graft (spinal fusion) to maintain the spine’s strength.
- Laminotomy. This procedure removes only a portion of the lamina, typically carving a hole just big enough to relieve the pressure in a particular spot.
- Laminoplasty. This procedure is performed only on the vertebrae in the neck (cervical spine). It opens up the space within the spinal canal by creating a hinge on the lamina. Metal hardware bridges the gap in the opened section of the spine.
-
Minimally invasive surgery. This approach to surgery removes bone or lamina in a way that reduces the damage to nearby healthy tissue. This results in less need to do fusions.
While fusions are a useful way to stabilize the spine and reduce pain, by avoiding them you can reduce potential risks, such as post-surgical pain and inflammation and disease in nearby sections of the spine. In addition to reducing the need for spinal fusion, a minimally invasive approach to surgery has been
If you are experiencing spinal stenosis, call us today to visit a spine surgeon nearest you, at 888-409-8006. Offices conveniently located in South Florida; Boca Raton, Deerfield Beach & Plantation.
